The Health IT Triad: HITECH, MACRA, and Cures
The policy trio driving the federal digital health transformation
Over the past decade, the healthcare industry has experienced a tremendous shift towards digitization, with healthcare providers and organizations embracing electronic health records, telemedicine, and other digital technologies. Though the private sector innovations in this space have been publicly visible, the policy initiatives driving these digital outcomes are more obscure.
By understanding the policy levers driving innovation and regulation in this space, we can see how various components of the federal government work together to certify, regulate, and build the health tech products we interact with every day.
In this post, we are going to describe how the 2009 Health Information Technology for Economic and Clinical Health Act (HITECH), the 2015 Medicare Access and CHIP Reauthorization Act (MACRA), and the 2016 21st Century Cures Act have played a significant role in driving the federal digital health transformation.
2004: Creation of the ONC
To understand how the health IT transformation started, we need to go back to 2004. In his State of the Union address, George W. Bush highlighted the importance of “computerizing health records [to] avoid dangerous medical mistakes, reduce costs, and improve care”. Following on this promise, he signed Executive Order (EO) 13335, which created the Office of the National Coordinator for Health IT (ONC) - igniting a chain reaction to help the US become a key player in the health IT world.
The mandate of the ONC as defined in EO 13335 is simple: to provide leadership for the development and nationwide implementation of an interoperable health information technology infrastructure to improve the quality and efficiency of health care. This EO has incentivized clinicians and hospitals to move away from paper records and rapidly digitized our healthcare delivery system.
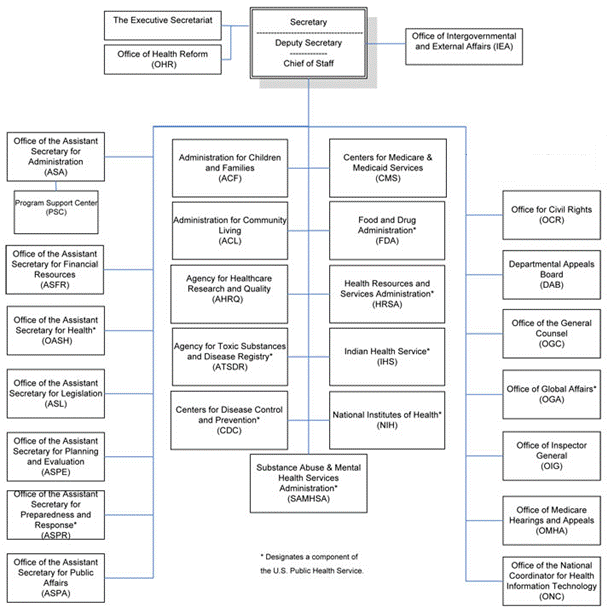
The ONC was developed as a new office under Health and Human Services, placing them in a strategic position to collaborate with other executive branch agencies and HHS departments. Today, the ONC continues to coordinate efforts with the Centers for Medicare and Medicaid Services (CMS), the National Institutes of Health (NIH), and more.
2009: HITECH Act
After the 2008 recession, Congress passed the American Recovery and Reinvestment Act (ARRA). This $787 billion stimulus package was signed by President Barack Obama in 2009 to create new jobs, modernize our nation’s infrastructure, and prevent further economic deterioration. Under Title XIII of the ARRA, you will find the Health Information Technology for Economic and Clinical Health (HITECH) Act.
With the HITECH Act, Congress appropriated around $25.8 billion for health information technology investments and incentive payments. The HITECH Act incentivized the use of EHRs by promising Medicaid payments for eligible professionals. Under Division B in Title IV, you will find the following language:
(I) For the first payment year for such professional, $15,000 (or, if the first payment year for such eligible professional is 2011 or 2012, $18,000).
(II) For the second payment year for such professional, $12,000.
(III) For the third payment year for such professional, $8,000.
(IV) For the fourth payment year for such professional, $4,000.
(V) For the fifth payment year for such professional, $2,000.
(VI) For any succeeding payment year for such professional, $0.
Eligible professionals who met the EHR criteria could earn up to $63,370 in Medicaid payments over 6 years and $44,000 in Medicare payments over 5 years. However, this funding was contingent on physicians demonstrating the “meaningful use” of their EHRs. Physicians could demonstrate “meaningful use” by showing that their EHR promotes electronic exchange, improves care coordination, ensures privacy and security of health data, and improves population and public health. Physicians that failed to adopt an EHR by 2015 would face a penalty of up to 1% of their Medicare payments.
The ARRA also allocated $2 billion in funding to the ONC to carry out the clauses in the HITECH ACT. Moreover, this act also introduced several privacy provisions that strengthened HIPPA. Entities that are covered by HIPPA are required to report data breaches that affect 500 or more people to the HHS or face steep financial penalties (up to $1.5 million!).
Before the HITECH Act was signed into law, only about 10% of healthcare organizations used Electronic Health Record (EHR) systems. Additionally, HIPAA-covered entities were not investing in privacy and security compliance because it was cheaper to just pay a financial penalty. After the HITECH Act, healthcare organizations were encouraged to transition to EHRs and invest in HIPPA compliance. Today, more than 95% of hospitals have an EHR. It’s no surprise that we almost take them for granted!
2015: MACRA Act
Congress passed the Medicare Access and Children's Health Insurance Program (CHIP) Reauthorization Act (MACRA) in 2015. To understand why Congress passed MACRA, we need to take a few steps back and talk about how Medicare pays physicians.
Medicare operates under a fee-for-service model. Under this system, Medicare determines a base rate for a specific service like a telehealth appointment or cancer screening. Medicare increases or decreases its payment to a provider based on variables like geographic location, patient complexity, and more.

One issue with the fee-for-service model is that physicians are incentivized to increase the volume of services they provide to get more money from Medicare over the quality of care they provide. This problem was exacerbated by a Medicare regulation called the Sustainable Growth Rate (SGR) formula. Simply put - if physicians spent too much money on healthcare services, then their overall Medicare payments were reduced. These payment cuts were directly tied to economic performance. In the late 90s, SGR led to increases in physician payments because of increased economic growth. But in 2002, the SGR rule caused a 4.8% cut in physician payments due to declining economic conditions and the looming cuts got worse every year after…
After the introduction of MACRA, the SGR rule was repealed and reduced this burden on physicians. MACRA also introduced two new programs to reward and incentivize physicians for value over volume. Under MACRA’s Merit Based Incentive Payments System (MIPS), physicians receive Medicare payment bonuses, penalties, or nothing based on total score from 4 categories: Quality, Resource Use, Clinical Practice Improvement Activities, and Meaningful use of certified electronic health records (EHR) technology.
Through the incorporation of EHR use in MACRA’s MIPS program, providers were now incentivized under a new system to receive potential payment bonuses for their use of ONC-certified health information technology.
2016: 21st Century Cures Act
The increase in EHR use from HITECH and MACRA was a huge step in modernizing our health IT infrastructure. EHR vendors like Epic, Cerner, athenahealth, and more were thriving in this market of selling their products to major providers and hospital systems. Unfortunately, many EHR vendors and developers were engaging in a practice called “information blocking.”
Information blocking describes the act of actively interfering with the process of sharing information between health record systems. For example, Epic has been known to oppose sharing its data with external applications and software that would benefit doctors and patients. Companies like Epic could prevent patients from accessing their own health information and sharing it with other providers who may use other types of EHR software.
The incompatibility between EHR systems was becoming a big problem for patients and providers by preventing access to medical histories. To solve this challenge, the 21st Century Cures Act was passed in 2020 to mandate the free flow of information or “interoperability” between health record systems. The prohibition of information blocking promoted the development of application programming interfaces (APIS) that would enable the passage of data between electronic health systems.
The 21st Century Cures Act has led to the development of global data standards for health data sharing like HL7 Fast Healthcare Interoperability Resources (FHIR) to create a common language between EHRs. This Act was critical to creating a health IT network that mandates the free flow of health data and information exchange.
Conclusion
The foresight and due diligence of health IT advocates for over two decades have enabled the widespread use of EHRs in medicine today. The health IT policy triad - HITECH, MACRA, and Cures - are critical drivers of the federal digital health transformation. Though the challenges facing EHR use and interoperability have not been fully resolved, our health information networks are continuously improving every day to serve the health needs of patients across the nation.